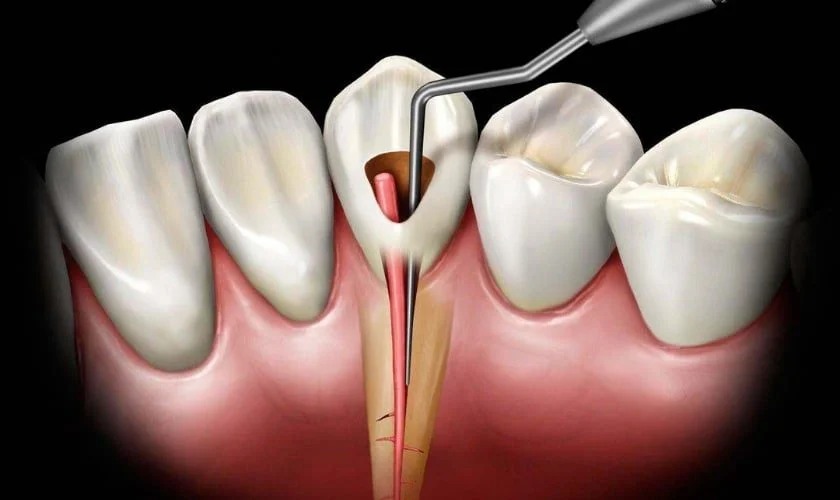
What Is Gum Disease?
Gum disease, or periodontal disease, is an infection of the gums and supporting structures of the teeth. It starts as gingivitis (mild inflammation) and can progress to periodontitis, causing tissue and bone loss.
Early detection is critical to prevent tooth loss and maintain overall health.
Signs and Symptoms
Red, swollen, or bleeding gums
Persistent bad breath
Receding gums
Loose or shifting teeth
Pain while chewing
Patients in Sydney should watch for these signs and visit a dentist promptly.
Causes of Gum Disease
Poor oral hygiene
Smoking or tobacco use
Genetic predisposition
Hormonal changes (pregnancy, menopause)
Diabetes and other systemic conditions
Holistic Effects of Gum Disease
Gum disease is not just a dental problem—it affects overall health:
1. Cardiovascular Health
Chronic inflammation from gum disease can increase the risk of heart disease, stroke, and high blood pressure.
2. Diabetes Management
Gum disease can make blood sugar harder to control, worsening diabetes.
3. Pregnancy Complications
Periodontitis may contribute to preterm birth and low birth weight.
4. Respiratory Health
Bacteria from infected gums can travel to the lungs, potentially worsening pneumonia or chronic respiratory disease.
5. Mental Health & Quality of Life
Chronic pain, tooth loss, and aesthetic concerns can lead to stress, low self-esteem, and social anxiety.
Prevention and Treatment
Prevention Tips
Brush twice daily and floss
Regular dental check-ups and cleanings
Quit smoking or tobacco use
Maintain a balanced diet rich in vitamins
Manage chronic conditions like diabetes
Treatment Options
Professional cleaning (scaling and root planing)
Antibiotic therapy for infection
Periodontal surgery in advanced cases
Laser therapy for targeted gum treatment
Final Thoughts
Gum disease is more than a dental issue—it’s a systemic health concern. Maintaining good oral hygiene and regular dental visits can prevent serious complications and improve overall health. Patients in Sydney should take gum health seriously to protect both their smile and their body.